What are eating disorders?
Lesson 1
What do the following celebrities all have in common?
Lady Gaga, Demi Lovato, Camila Mendes, Kesha, Gabourey Sidibe, and many others have all been candid about their struggles with body dysmorphia and their eating disorders.
The Taylor Swift documentary is the latest to join the ranks of celebrities who have publicly discussed their eating disorder — talking about food in terms of reward and punishment.
Being in the public eye can be difficult and always under the scrutiny of the press and media can take its toll.
Unfortunately, this is not a new concept, and the love and hate relationship with the national press and media has been around since the dawn of time.
Here are a few from the past, before this condition was fully understood.
Karen Carpenter (The Carpenters') was taking ipecac syrup to induce vomiting but had unknowingly dissolved her own heart muscle with this syrup. She was only 32 when she died from Anorexia Nervosa.
Judy Garland in the “Wizard of Oz” didn’t have a fairy tale ending, she was constantly bullied and criticised continuously by film executives who believed that she was physically unattractive and manipulated her on-screen physical body appearance with sily weight-loss diets
Her lifelong eating disorder arguably fuelled her drug addiction, eventually led to her death in London from an accidental barbiturate overdose at age 47.
The social media problem is only escalating, Caroline Flack was found dead in February 2020 from a suicide, amongst her own relationship problems and a previous battle with depression, for which she needed medication. She had to endure vile negative comments, attacking her emotionally with loss of self-esteem and leaving her in a more vulnerable state.
Body shaming by internet trolls are only fuelling this concept and can be a source of anxiety and also hurt deeply for many individuals; with or without any celebrity status.
Diagnostic tools
Eating disorders are serious mental health conditions and every 62 minutes someone dies as a direct result of an eating disorder. Four eating disorders are currently recognised in the International Classification of Diseases (ICD – 10) and the Diagnostic and Statistical Manual of Mental Disorders (DSM – 5), and although they can affect anyone, they are most common in females.
Types of eating disorders
We shall start with the most common types and then move into the unique forms of this disease which fall under this classification to give an overall perspective of the aetiology, symptoms, and mindset you may encounter in different individuals.
The following are the most common forms of eating disorders, and they include anorexia nervosa, bulimia nervosa, binge-eating disorder, and avoidant restrictive food intake disorder (ARFID). This term replaces what was known as a "feeding disorder of infancy and early childhood," a diagnosis previously reserved for children under seven years old.
Although ARFID generally develops during infancy or early childhood, it can persist into adulthood. What is more, it is equally common among men and women.
Eating disorders are a range of psychological conditions that cause unhealthy eating habits to develop. They might start with an obsession with food, body weight, or body shape.
Although there are common signs and symptoms, any two individuals with the same eating disorder can have somewhat different experiences.
Overview of eating disorders
These conditions can affect their physical and mental well-being, often leading to severe and even deadly medical emergencies.
Eating disorders often co-occur with other mental health conditions like depression, anxiety, obsessive-compulsive disorder, and substance abuse.
Approximately 20 million American women will have developed at least one type of eating disorder at some point in their lives, and perhaps more than one; and 10 million men having or have had an eating disorder at some point in their life. Statistically, females are twice as likely as males to have an eating disorder.
Eating disorder, are most commonly associated with young, caucasian women between the ages of 12 and 35, many of whom are athletic.
Nevertheless, be careful of stereotyping individuals because eating disorders do not discriminate between anyone, rich or poor, young or old, and of any race, ability, culture, gender or sexual orientation can develop an eating disorder.
Eating disorders may be caused by a variety of factors.
Mental illness, (anxiety, Depression, OCD, Personality disorders, Substance Misuse) Past trauma (PTSD, bullying, sexual assault) Temperament and Genetics have a strong association in acquiring an eating disorder. One of the strongest contenders is genetics, with some evidence in twins studies and genetic markers, have indicated that eating disorders may be hereditary.
A study in 2016 by Prof. Gorwood, head of the Clinic for Mental and Brain Diseases, stated that anorexia nervosa is a highly transmissible disorder (70%). One of the genes most often associated with anorexia nervosa codes for BDNF, a factor involved in neuron survival and neuroplasticity.
Perhaps the most controversial points on his research paper was the theory that anorexia nervosa might not be explained by the fear of gaining weight, but rather by the pleasure of losing it, and that the phenomenon might be genetically influenced. The work challenges the notion of fear of weight gain in anorexia patients is the main driving force.
Obviously, this challenges one of the main criteria and current thinking in anorexia patients: Being an intense fear of becoming fat. It could also impact on the way we approach treatment for this group in the future. (Anorexia nervosa: Pleasure at getting thin more than fear of getting fat)
Eating disorders in non-Western cultures.
Perhaps it is best to point out that Non-fat phobic anorexia nervosa has been observed in non-Western countries cultures before western influences. For example, in Hong Kong, eating disorders were also seen from the 1990s onward and showed features commonly associated with Western eating disorders were absent, such as body dissatisfaction.
Typically individuals attributed their restrictive food intake to somatic complaints (i.e., bloating, abdominal pain, or just not hungry and it was termed “Non-Fat Phobic Anorexia Nervosa".
Fiji is a country that has been heavily studied due to the rise in eating disorders after Westernisation influence started in the mid-1990s. Prior to the 1990s, there was only one documented case of an eating disorder.
In the mid-1990s, television was introduced into Fiji society, and researcher Dr Becker leading various studies on measuring eating psychopathology and beauty ideals both before and after the introduction to television.
Once television arrived, rates of eating disturbances escalated among the Fijian women. With the prevalence of television and more westernised ideas, rates of body dissatisfaction, dieting, desire to lose weight and the thin ideal internalisation as well as bulimic behaviours became more widespread across the island.
Personality traits
In patients with anorexia nervosa, Personality traits are another cause. In particular, neuroticism, perfectionism, and impulsivity are three personality traits often linked to a higher risk of developing an eating disorder.
Obsessive-compulsive disorder (OCD) and eating disorders
There are also similarities between obsessive-compulsive disorder (OCD) and some forms of eating disorders in which the obsession is focussed around body image and the compulsion around food-related behaviour.
Neurotransmitters and brain pathology
More recently, experts have proposed that differences in brain structure and biology may also play a role in the development of eating disorders. More specifically, the researchers found low serotonin binding among people with obsessive-compulsive disorder (OCD) and social anxiety disorder. Therefore, resulting in less available serotonin in the brain.
The “serotonin hypothesis” of clinical depression is almost 50 years old. At its simplest, the hypothesis proposes that reduced activity of serotonin plays a causal role in the pathophysiology of depression.
Unfortunately, this simple biochemical theory that once linked low levels of serotonin with depressed mood is no longer tenable. However, experimental and computational accounts of how serotonin influences emotional processing throw an intriguing light on the neuropsychology of depression and its pharmacological treatment in the future.
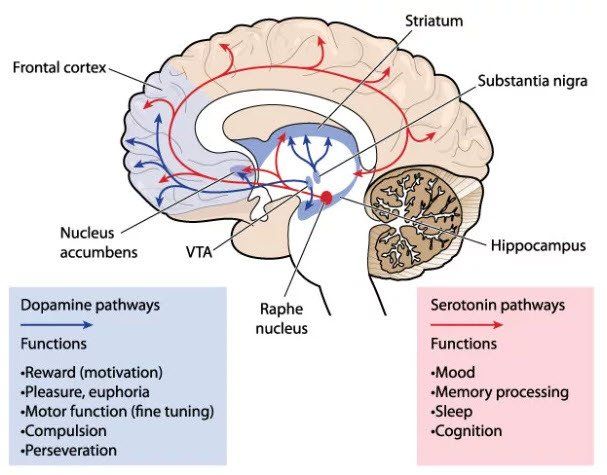
Both dopamine and serotonin play a role in depression, though experts are still trying to figure out the details. In particular, levels of the brain messengers serotonin and dopamine may be critical factors, but more studies are needed before any strong conclusions can be made.
There’s a close link between dopamine and how you experience a pleasure and any dysfunction of the dopamine system might also contribute to bipolar disorder and schizophrenia. Serotonin affects emotional processing, which can have significant effects on mood. (food addiction / reward and reinforcement)
Social Media influence
Epidemiological studies show how psychology within eating disorders are influenced by social media and peer pressure with perceived pressures to be thin, cultural preferences for thinness, and exposure to media promoting such standards in magazines and films as normal.
Peer pressure (or social pressure) is the direct influence on people by peers, or the effect on an individual who gets encouraged to follow their peers by changing their attitudes, values or behaviours to conform to those of the influencing group or individual. This can result in either a positive or a negative effect or both.
Family values
Families pressure also contribute, too; parents who emphasise looks, encourage dieting or criticise their children's bodies may be more likely to raise a child with an eating disorder. In fact, certain eating disorders appear to be mostly nonexistent in cultures that have not been exposed to Western ideals of thinness.
The prevalence of eating disorders in non-Western countries is lower than that of the Western countries but appears to be increasing. (A Comparison of Western and Non-Western Countries (2004) )
Eating disorders and depression
Presently, there are two predominant hypotheses on the relationship between eating disorders and depression. The first hypothesis states that bulimia nervosa is an affective variant of depression. This idea came about due to early reports of a high prevalence of clinical depression in bulimics and a high lifetime prevalence of depression in the families of these patients.
Recent studies, however, provide evidence that this type of relationship between bulimia and depression is still unconfirmed. The second hypothesis constitutes that bulimia is a “distinctive diagnostic entity with a psychopathological process different from that of other mental disorders.”
Moreover, results of a small study suggest that women with eating disorders who have attempted suicide may have had a depressive disorder long before their problems with food began. Researchers also found that among 27 eating disorder patients with a history of suicide attempts, two-thirds had major depression before the onset of the eating disorder.
That compares with just one of 27 patients who had never attempted suicide. Women in the suicidal group also developed depression and anxiety disorders at a younger age than the other women did. A substantial number of people with eating disorders purposely injure themselves or attempt to take their lives, according to the study.
The findings suggest that for most people with eating disorders and no history of suicidal behaviour, depression may be a consequence of the eating disorder. However, for those who are suicidal, the first and perhaps most “central” psychological problem may often be significant depression.
Therefore, people with eating disorders and a history of depression may be at increased risk for suicide. This, they note, suggests the need to put more emphasis on regulating emotion and reward (dopamine) and mood (serotonin) in treating these patients.
Anorexia Nervosa
Despite eating disorders having the highest mortality rate of any mental illness, most people cannot tell when someone close to them is living with one.
Anorexia nervosa encompasses behaviours like dieting, fasting, over-exercising, taking diet pills, diuretics, laxatives and vomiting.
It is especially prevalent among young to middle-aged women and outnumbers men affected by anorexia, drastically. However, it is increasing among young men annually. Anorexia is often accompanied by an inability on the person's part to appreciate the severity of the situation (i.e. they do not see themselves as being unwell).

Symptoms of anorexia nervosa
The Diagnostic and Management Guidelines for Mental Disorders in Primary Care, ICD-10 requires the following symptoms for a diagnosis of anorexia:
- Weight loss (or lack of weight gain in children), leading to a weight that is too low - Maintaining a body weight that is at least 15 per cent below the national average for their age and height. Weight loss is brought about by inadequate food intake with the person avoiding 'fattening' foods.
- Preventing weight gain may also involve self-induced vomiting, self-induced purging
- Excessive exercise or use of appetite suppressants and/or diuretics.
A self-perception of being too 'fat', with an intense fear of weight gain and obsession with weight leads to this persistent behaviour to prevent weight gain/promote weight loss.

A normal hormonal function is affected, with the absence of periods in women and loss of sexual interest in men. (Exceptions for this are where anorexia develops before puberty, in which case puberty may be delayed, or in women who take the contraceptive pill which may maintain their periods artificially.) Missing at least three menstrual cycles consecutively.
However, 'atypical' anorexia can also be diagnosed where some of these elements may be missing, dependent on a professional medical assessment.
People with anorexia nervosa avoid food, severely restrict food, or eat minimal quantities of only certain foods. Even when they are dangerously underweight, they may see themselves as overweight. They may also weigh themselves repeatedly.

There are two subtypes of anorexia nervosa: a restrictive subtype and binge-purge subtype.
Restrictive: People with the restrictive subtype of anorexia nervosa place severe restrictions on the amount and type of food they consume.
Binge-Purge: People with the binge-purge subtype of anorexia nervosa also place severe restrictions on the amount and type of food they consume. Besides, they may have binge eating and purging behaviours (such as vomiting, use of laxatives and diuretics, etc.).
It is essential to seek treatment early for eating disorders. People with eating disorders are at higher risk for suicide and medical complications. Some people with eating disorders may also have other mental disorders (such as depression or anxiety) or problems with substance use.

Ongoing treatment for health problems
Eating disorders can cause serious health problems related to inadequate nutrition, overeating, bingeing and other factors. The type of health problems caused by eating disorders depends on the type and severity of the eating disorder. In many cases, problems caused by an eating disorder require ongoing treatment and monitoring. They may need to be hospitalised in order to keep them safe.
Anorexia can be fatal.
Anorexia nervosa has the highest mortality (death) rate of any mental disorder. People with anorexia may die from medical conditions and complications associated with starvation; by comparison, people with others eating disorders die of suicide. It is the third most common chronic illness among teenage girls with a mortality rate 12 times higher than the death rate for all causes of death for females 15-24 years old. (American Journal of Psychiatry, March 2017)
Health problems linked to eating disorders may include:
Electrolyte imbalances, which can interfere with the functioning of your muscles, heart and nerves - Electrolyte imbalance (too low or too high levels of sodium, calcium, potassium and other minerals), which can lead to stroke or heart attack
Heart problems
- Low blood pressure - slowed breathing and pulse (anorexia)
- High blood pressure (binge eating)
- Irregular heartbeats -heart failure (bulimia)
Digestive problems (inflammation /damage to the oesophagus/throat due to stomach acid released
Nutrient deficiencies - Lethargy, sluggishness, or feeling tired all the time
Dental cavities and erosion of the surface of your teeth from frequent vomiting
Low bone density (osteopenia or osteoporosis) as a result of irregular or absent menstruation or long-term malnutrition
Stunted growth caused by poor nutrition (anorexia)
Mental health conditions such as depression, anxiety, obsessive-compulsive disorder or substance abuse
Lack of menstruation and problems with infertility and pregnancy (amenorrhea triggered by anorexia)
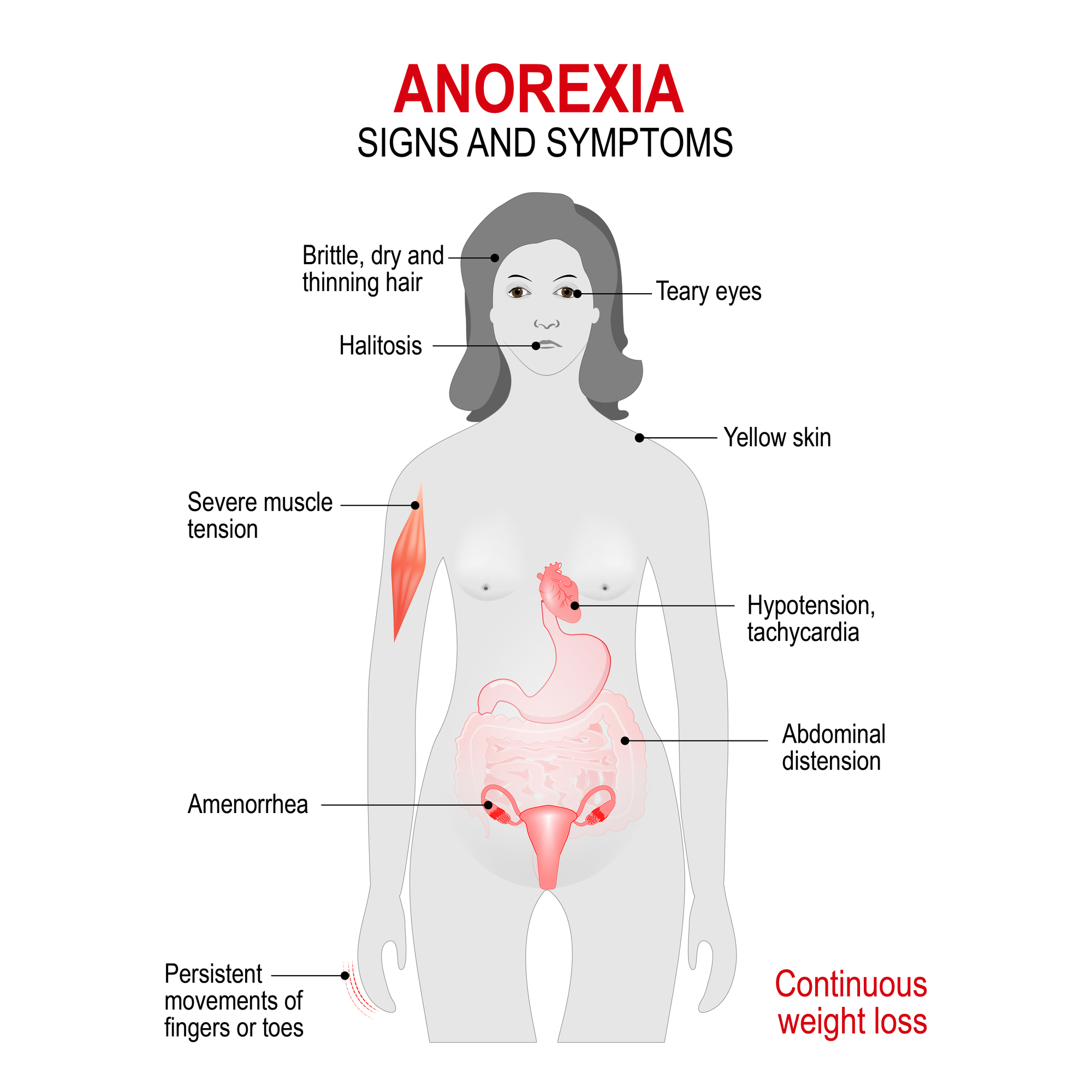
A relentless pursuit of thinness and unwillingness to maintain a normal or healthy weight (emaciation)
Brittle hair and nails
Dry and yellowish skin
Growth of fine hair all over the body (lanugo)
Severe constipation
Drop-in internal body temperature, causing a person to feel cold all the time
Body dysmorphic disorder (BDD)
What is bulimia nervosa?
People with bulimia nervosa have recurrent episodes of eating unusually large amounts of food and feeling a lack of control over these episodes. This binge-eating is followed by behaviours that compensate for the overeating, such as forced vomiting, excessive use of laxatives or diuretics, fasting, excessive exercise, or a combination of these behaviours.

Unlike those with anorexia nervosa, people with bulimia nervosa may maintain a healthy weight or be overweight.
Warning signs specific to bulimia nervosa
Evidence of purging behaviours, e.g. frequent visits to the bathroom during/ after meals, signs or smells of vomiting, presence of laxatives or diuretics
Swelling of the cheeks or jaw area or calluses on the back of the hands and knuckles due to self-induced vomiting
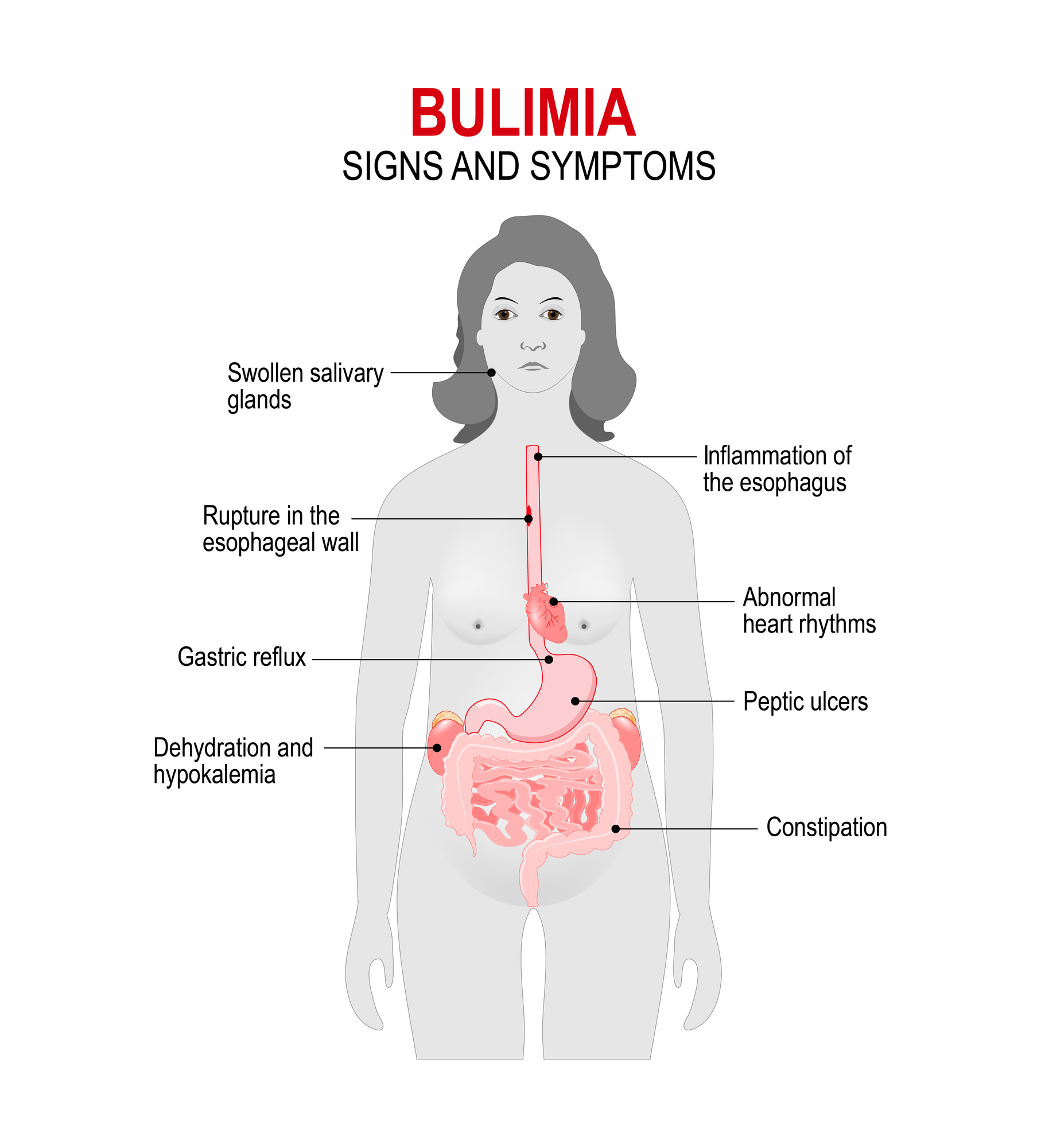
Discoloured or stained teeth (effect from stomach acid during vomiting)
Dramatic weight loss is possible but not necessarily always the case. Nevertheless, the person's self-perception may not seem to reflect their weight accurately, even if healthy (i.e. they see themselves as much 'fatter' than others do).
What is binge-eating disorder?
People with binge-eating disorder lose control over their eating. Unlike bulimia nervosa, periods of binge-eating are not followed by purging, excessive exercise, or fasting. As a result, people with binge-eating disorder are often overweight or obese.

Binge eating symptoms include:
Eating unusually large amounts of food in a specific amount of time, such as a 2-hour period
Eating fast during binge episodes
Eating even when full or not hungry
Eating until uncomfortably full
Eating alone or in secret to avoid embarrassment
Feeling distressed, ashamed, or guilty about eating
Frequently dieting, possibly without weight loss.
Symptoms of binge eating disorder
To qualify for binge eating disorder, the following symptoms need to be present:
Repeated episodes (at least once a week for 3 months) of binge eating, during which the person:
Eats significantly larger than normal amounts of food in a short period of time (compared to what most people would consume)
Feels out of control about their eating, i.e. they feel they cannot stop eating or control what or how much they are eating, although they may want to.
Binge eating episodes are also associated with three (or more) of the following:
Eating much more rapidly than normal
Eating when not feeling physically hungry
Eating alone/hiding the binges because of feelings of shame
Feeling disgusted, depressed or very guilty about the binge afterwards
The person is clearly distressed by their binges.
There are no compensating behaviours as in bulimia nervosa.

Physical health problems linked with binge eating disorder
The main physical health consequence of binge eating disorder is an increase in weight and associated risks. It is important to note that most people who are obese do not have binge eating disorder. However, most people with binge eating disorder have a normal or above-average weight, with many being obese.
Physical health risks are, therefore associated with obesity and may include:
High blood pressure
High cholesterol levels
Heart disease
Type II diabetes
Gallbladder disease
Fatigue
Joint pain
Sleep apnea
As with bulimia nervosa, there is some risk of gastric rupture during a binge
Avoidant Restrictive Food Intake Disorder (ARFID)

Some children, however, are extremely picky. They may try to limit themselves to only a few foods. They may avoid all foods of a certain colour, texture, smell or category. They might be restrictive enough that it's hard for them to gain any weight or continue to grow normally.
Lack of interest or other avoidance of food due to the sensory characteristics of food, such as colours and textures.
Avoidance is associated with at least one of the following:
- Significant weight loss or, in children, failure to reach expected weight and height
- Significant nutrient deficiency
- Dependence on nutritional supplements or oral feeding tube
- Disruption of psycho-social functioning
The condition cannot be explained away by the unavailability of foods or culturally approved eating practices.
Unlike more well-known eating disorders of childhood and adolescence, ARFID kids are not avoiding eating due to any concern with body image. They are not trying to lose weight.
In addition, unlike anorexia and bulimia where a child ate normally and then later develops the eating disorder, ARFID usually starts in young childhood and continues as kids get older, sometimes getting worse.
There are no issues with bodyweight or body image and avoidance is not associated with anorexia or bulimia.
There is no other eating disturbance or medical condition present that would explain the avoidance, or the avoidance is more extreme than would typically be associated with another condition.
Teenager developed permanent sight loss after living on a diet of chips and crisps
Eye doctors in Bristol cared for the 17-year-old after his vision had deteriorated to the point of blindness.
Since leaving primary school, the teen had been eating only French fries, Pringles and white bread, as well as an occasional slice of ham or a sausage.
Tests revealed he had severe vitamin deficiencies and malnutrition damage.
Extreme picky eater
The adolescent had seen his GP at the age of 14 because he had been feeling tired and unwell. At that time he was diagnosed with vitamin B12 deficiency and put on supplements, but he did not stick with the treatment or improve his poor diet.
Three years later, he was taken to the Bristol Eye Hospital because of progressive sight loss, Annals of Internal Medicine journal reports.
Dr Denize Atan, who treated him at the hospital, said: "His diet was essentially a portion of chips from the local fish and chip shop every day. He also used to snack on crisps - Pringles - and sometimes slices of white bread and occasional slices of ham, and not really any fruit and vegetables.
"He explained this as an aversion to certain textures of food that he really could not tolerate, and so chips and crisps were really the only types of food that he wanted and felt that he could eat."
He was not over or underweight, but was severely malnourished from his eating disorder - avoidant-restrictive food intake disorder.
He had lost minerals from his bone, which was really quite shocking for a boy of his age.
He was put on vitamin supplements and referred to a dietitian and a specialist mental health team.
In terms of his sight loss, he met the criteria for being registered blind.
ARFID & AUTISM
Feeding and eating problems are common autistic individuals. Difficulties such as only eating a very few foods, going a long time without eating and extreme anxiety about foods and mealtimes are frequently reported. These problems are not always understood and as a result, parents/carers and the individuals themselves often report feelings of stress, helplessness and blame.
For some, these problems can be managed relatively easily with the right support, for others the eating issues can have a lasting and debilitating impact leading to weight loss and/or malnutrition, increased social withdrawal and stigma. Very positively many autistic people now meet the criteria for an additional diagnosis of ARFID. This can lead to a better understanding of the eating challenges and more support and professional help.
IS ARFID DIFFERENT IN AUTISTIC PEOPLE?
There are many similarities in the eating patterns of autistic people with ARFID and those who have ARFID but no additional autism. These include: Sensory sensitivities, high anxiety around foods/eating situations and lack of interest in food. However, in autistic individuals (both children and adults) these issues can be more severe and more resistant to treatment.
This is simply due to the additional difficulties and differences having autism places on the person. For example, sensory issues can be heightened and more complex; routines and rituals around foods can be more inflexible and rigid due to additional anxiety about change and the autistic person often has more problems recognising and responding to internal body states such as hunger or being full (known as ‘interoception’).
Autistic people also have extra difficulties communicating and interacting with others (often called ‘social-communication’ difficulties). This means it can be harder for them to explain their difficulties with food, it can be harder for family and friends to understand and manage the issues and harder for the individual to participate in treatment, particularly if this is offered in a group or is a ‘talking therapy’.
WHAT OTHER EATING PROBLEMS MIGHT AUTISTIC PEOPLE HAVE?
In addition to having an ARFID style pattern of eating it is increasingly recognised that autistic individuals are at risk of developing other eating problems or disorders such as Anorexia Nervosa (AN) or Bulimia Nervosa (BN).
Typically these eating disorders often appear for the first time in adolescence or early adulthood (whereas ARFID is often more obvious in earlier childhood) and often lead to serious weight loss and other physical and mental health problems. For more information about these types of eating problems and where to find support see: www.beateatingdisorders.org.uk
Given that these type of eating disorders are generally more common in females; autistic girls and women appear to be more at risk. In addition, for some autistic girls and women controlling eating is a way of managing overwhelming feelings of anxiety.
This can be particularly true during adolescence where physical changes such as puberty and social and academic pressures can cause anxiety to spiral out of control. As a result, it is very important that such anxiety and associated eating problems are recognised early and given the right support.
For more information about these types of eating problems and where to find support see:
https://network.autism.org.uk/good-practice/evidence-base/anorexia-nervosa-autistic-females
In addition to having ARFID some autistic people display ‘Pica’ which is the medical term for eating non-foods. Commonly eaten items include: Paper, cloth, wood, plastic, stones, earth, metal and faeces. Pica carries serious health risks with only 1 episode having the potential to lead to significant harm.
For more information about these types of eating problems and where to find support see: https://network.autism.org.uk/knowledge/insight-opinion/james-frankish-and-pica
We don’t know what causes pica and there may even be different types of pica behaviour. For autistic people managing sensory needs and supporting anxiety appear to be important as is controlling access, wherever possible, to potentially dangerous pica items. Doing so can help keep the individual safe and possibly even reduce the individual engaging in pica.
For more information about these types of eating problems and where to find support see: https://network.autism.org.uk/knowledge/insight-opinion/understanding-and-managing-pica
Other specified feeding or eating disorder (OSFED)
Anorexia, bulimia, and binge eating disorder are all diagnosed according to a list of expected behavioural, psychological, and physical symptoms. Sometimes a person’s symptoms do not exactly fit the expected symptoms for any of these three specific eating disorders. In that case, they might be diagnosed with an “other specified feeding or eating disorder” (OSFED). [Previously called Eating Disorder Not Otherwise Specified or EDNOS]
OSFED is every bit as serious as anorexia, bulimia, or binge eating disorder, and people suffering from OSFED are every bit as deserving and in need of treatment – their eating disorder is just presenting differently. It is common for symptoms to not fit with the exact diagnostic criteria for anorexia, bulimia, or binge eating disorder – OSFED accounts for a large percentage of eating disorders.
Some specific examples of OSFED include:
- Atypical anorexia – where someone has all the symptoms a doctor looks for to diagnose anorexia, except their weight remains within a “normal” range.
- Bulimia nervosa (of low frequency and/or limited duration) – where someone has all of the symptoms of bulimia, except the binge/purge cycles don’t happen as often or over as long a period of time as doctors would expect.
- Binge eating disorder (of low frequency and/or limited duration) – where someone has all of the symptoms of binge eating disorder, except the binges don’t happen as often or over as long a period of time as doctors would expect.
- Purging disorder – where someone purges, for example by being sick or using laxatives, to affect their weight or shape, but this isn’t as part of binge/purge cycles.
- Night eating syndrome – where someone repeatedly eats at night, either after waking up from sleep or by eating a lot of food after their evening meal.

Like any other eating disorder, OSFED is a very serious mental illness that is not only about the way the person treats food but about underlying thoughts and feelings. The eating disorder may be a way of coping with these thoughts, or a way of feeling in control.
People with OSFED may work to hide their illness and someone may have been ill for a long time before physical symptoms appear if they do at all.
Any of the symptoms associated with bulimia, anorexia, or binge eating disorder can be part of OSFED, and these would come with the same short-term and long-term risks that they present in the case of these specific eating disorders.
As with other eating disorders, it will probably be changed in the person’s behaviour and feelings that those around them notice first before any physical signs appear.
Midlife (Eating Disorder)
Ask anyone who is over 40 and has made the New Year’s resolution to lose five pounds, and they will tell you, it is a lot harder than when they were in their 20s. As metabolism starts to slow down, you can’t even maintain your weight with the same eating and exercise habits that worked in the past.
Hormone levels are part of the problem. —to use a scientific term—all over the place. Spikes in cortisol and dips in testosterone not only make you bloated, but you get the double-whammy of having no energy to work out. Furthermore, what starts as a diet or new workout routine can spiral out of control.
Midlife Stressors
Major transitions like divorce or having an empty nest for the first time can cause vulnerability and that can trigger an eating disorder. When life feels out of control, strict adherence to a diet and counting calories can morph into an eating disorder.

Eating disorder relapse
It is not uncommon for an eating disorder to recur. Some women may have had anorexia or bulimia when they were teenagers or young adults, but then it was resolved and they had a long period of good health, but during perimenopause and menopause—with all the physical and emotional changes—the eating disorder may return.
A study by the American Journal of Psychiatry examined female adolescents brain scans before and after treatment for anorexia, found that their brains still had an elevated reward system compared to participants without the eating disorder. This disorder fundamentally changes the brain response to stimuli in our environment and the brain may not fully return to the normal state.
This study showed that the reward system was elevated when the patients were underweight and remained so once the weight was restored.
The neurotransmitter dopamine might be the key, researchers said, which was previously discussed under depression and eating disorders.
It’s Often Undetected
Since these women do not fit the stereotype, even doctors often miss the warning signs; and friends and family misjudge the symptoms. When a woman in her 30s or 40s develops an eating disorder, she may be caring for children, holding down a job, and maybe even caring for elderly parents. With so much going on, she can get away to some degree with having an eating disorder and no one will notice until it becomes severe.
Orthorexia Nervosa
Orthorexia is an unhealthy obsession with "healthy" eating. Here's a guide to a less common type of disordered eating.
When you think of healthy eating, it probably conjures up ideas of balanced diets, fresh fruits and vegetables, whole grains, limited processed foods, and beneficial lifestyle choices, like choosing to eat organic foods, avoid chemical food additives and support sustainable agriculture, whenever possible.
What if I told you that for some people—those who take the idea of healthy eating to an extreme—such a lifestyle can lead to a borderline form of eating disorder?
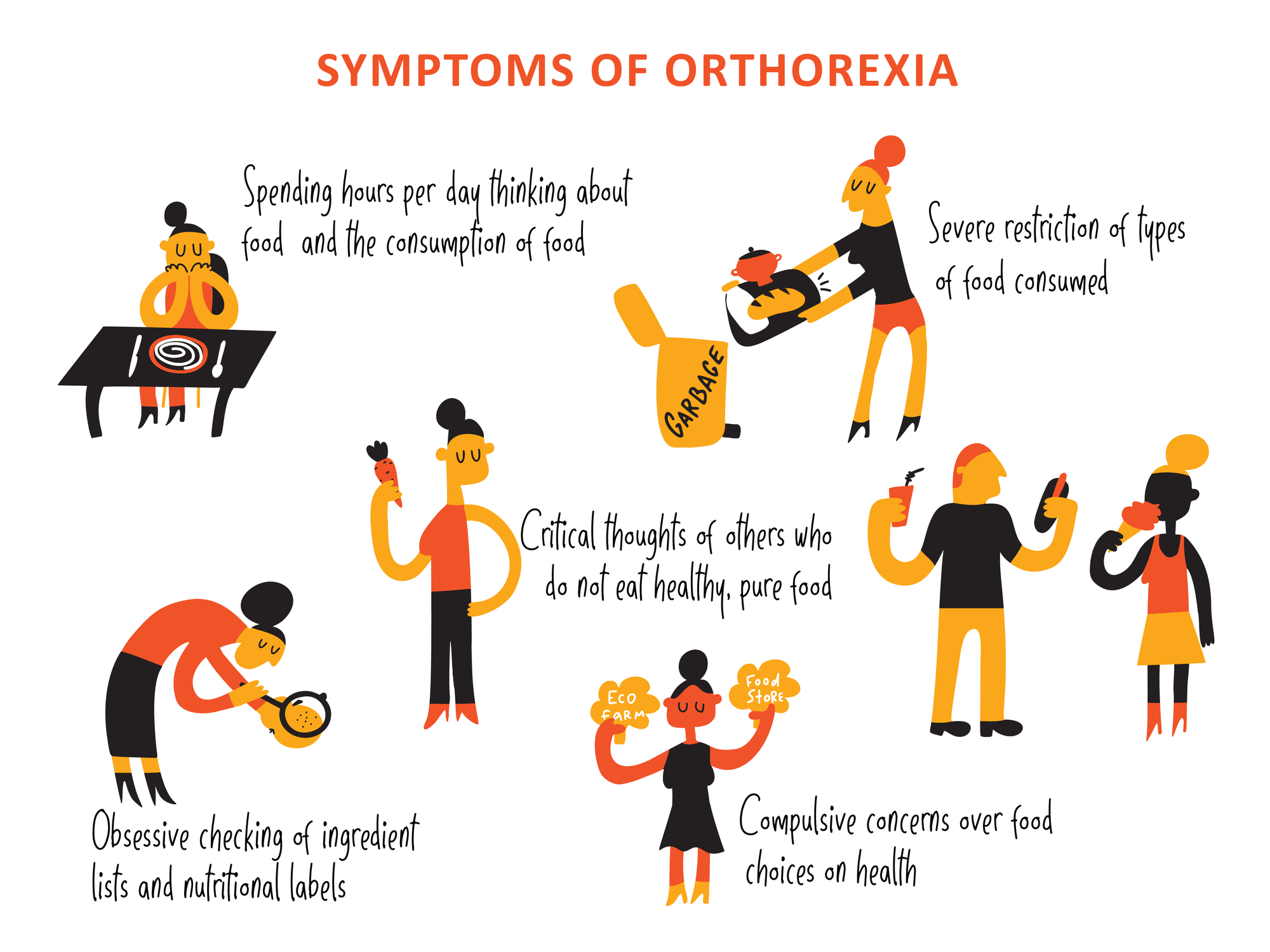
When Healthy Eating Becomes a Problem
Orthorexia Nervosa, a term coined by American physician Steven Bratman, MD in 1977, is characterized by an unhealthy obsession with the quality of foods in one’s diet.
From the Greek, the term orthorexia nervosa literally means “correct diet.” Since obesity stemming from too much sugar, fat, calories, and processing in the American diet is practically considered a national emergency, you might be wondering why or how any type of healthy eating could be a problem.
But of course, it’s not healthy eating in and of itself that is a problem. It’s a problem when a fixation on healthy eating turns seemingly positive lifestyle changes into a dangerous road of obsession over “pure” food consumption.
It’s a problem when it causes major disruptions to your well-being and social life. Malnutrition can result and, sometimes, heart issues and other problems associated with malnutrition may arise.
Social isolation and interference with interpersonal relationships occur when someone with orthorexia starts putting themselves on a “nutritional pedestal” and looking down on those who don’t follow the same restrictive lifestyle.
The term Orthorexia Nervosa is not officially recognized as an eating disorder in the Diagnostic and Statistical Manual of Mental Disorders (DAM-5) or by the American Psychiatric Association. Much research has been done on orthorexia, but the classification and definition of this condition is still being debated.
Physicians and mental health professionals may describe individuals living with orthorexia as possessing an unhealthy obsession with the quality of foods they consume but guidance and tools for diagnosing and treating the condition have not been standardised.
Orthorexia nervosa can easily go unnoticed because it does not seem unusual to be “obsessed” with healthy eating during a time when researchers, health professionals, food marketers, and media seem to constantly change the definition of a healthy diet.
Orthorexia nervosa also differs from more widely known and recognised eating disorders, such as Bulimia nervosa and Anorexia nervosa , that are characterized more by an unhealthy fixation on the amount of food consumed as well as weight and body image, than the condition or source of food eaten.
However, researchers have found that those who suffer from orthorexia share many of the same psychological and behavioral traits with those who suffer from other eating disorders.
The Symptoms of Orthorexia
Those who suffer from orthorexia nervosa are fueled by the desire to consume pure, healthy foods, obsessing over maintaining a perfect diet rather than an ideal weight. Someone with orthorexia may refuse to eat any food that contains anything they consider to be unhealthy or impure, such as artificial flavors, colors, or preservatives, fat, sugar, or salt, pesticides, genetically modified organisms, animal or dairy products. While this can be a normal approach to food for some people, if you are suffering from orthorexia your attitude and behavior toward eating a clean diet is obsessive and exaggerated.
You may:
Have obsessive thoughts over the effects of the food you eat on medical conditions, such as asthma, anxiety, allergies, or digestive disorders and including conditions that have not been diagnosed.
Severely restrict the types of food you eat because you deem so many foods acceptable to your diet.
Use significant amounts of probiotics, herbal remedies, and other supplements thought to have healthy effects on the body.
Have irrational concerns about preparation of foods, relating to food washing techniques and sterilization of utensils.
Experience strong emotional reactions to food, such as:
Feelings of satisfaction and happiness from clean, healthy, pure eating.
Feelings of guilt when consuming foods that are not considered healthy and pure.
Excessive time spent thinking about food and the consumption of food.
Regular advanced meal planning, feelings of guilt and displeasure when meals are not planned in advance.
Having critical, judgmental thoughts of others who do not follow healthy, pure eating plans.
Avoidance of eating food away from home or not prepared in your home kitchen, because you will not be able to comply easily with your healthy eating plan.
Avoiding food bought or prepared by others.
Creating distance between friends and family who do not share the same beliefs you have about food.
Compulsive behaviors
Depression
Anxiety
Mood swings
Feelings of shame
Self-loathing
Social isolation
When compulsive behaviors and mental preoccupations with healthy eating start to impair your quality of life, you may end up suffering from severe weight loss, malnutrition, or some other type of medical condition based on severe diet restrictions.
In addition, orthorexia may cause problems in your social, academic, or work life. If you are suffering from orthorexia, you may also suffer from negative self-worth, negative body image, and become obsessively dependent on your healthy eating lifestyle to the point of social isolation.
Self-Test for Orthorexia Nervosa
- If you recognize signs or symptoms of orthorexia nervosa in yourself, consider the following questions:
- Do you ever wish you could stop thinking so much about food and spend more time thinking about your loved ones?
- Are you constantly questioning food and considering how foods are unhealthy for you?
- Do you feel guilt or shame when you stray from your perfect diet?
- Does it seem physically impossible to eat a meal prepared by someone other than yourself?
- Do you feel “in control” when you stick to your planned, healthy, pure diet?
- Do you look down on others who eat less healthfully than you?
If you answered yes to several or all of these questions, speak with a doctor about your concerns. You can start with your primary care physician or mental health care provider if you have one, who can then refer you to a specialist, if necessary.
Treatment Options

There is no official treatment designed specifically for someone suffering from orthorexia but according to the National Eating Disorders Association, mental health care professionals often treat the condition similarly to anorexia or obsessive-compulsive disorder.
Psychotherapy can help you change their obsessive thought patterns about food and at the same time, treat any co-existing mental health conditions, such as depression, panic disorders, and stress and anxiety disorders. Regular sessions with your therapist will allow for reassessments and treatment plan changes, as needed.
Eating disorders and pregnancy

A study by University College London in May 2019 found women who had had an eating disorder at any point before childbirth, even if it was years earlier in adolescence, were more likely to experience depressive symptoms during pregnancy and up to 18 years after the birth of their child.
This study suggests that many people with eating disorders might not fully recover since we know that eating disorders and depression often happen at the same time.
Previous studies had suggested that depressive symptoms among mothers with eating disorders might improve after the perinatal period, but those studies did not have such a long follow-up time to confirm that the increased risk of depressive symptoms does persist for women who have had an eating disorder.
The research team found that women who had ever had anorexia nervosa or bulimia nervosa experienced more depressive symptoms over an 18-year follow-up than those who had never had an eating disorder.
(Prior eating disorders linked to long-term depression risk for mothers)
Rumination Disorder
What is rumination disorder?
Rumination disorder is an illness that involves repetitive, habitual bringing up food that might be partially digested. It often occurs effortlessly and painlessly and is not associated with nausea or disgust.
Rumination disorder can affect anyone at any age.
Vomiting in rumination disorder is different from the kind of sickness you might get with a stomach bug, for example – the person will not appear to feel sick or experience involuntary retching. The person may re-chew and re-swallow the food or just spit it out. People with rumination disorder often do not feel in control of their disorder.
The exact causes of rumination disorder are not known.
Other illnesses can cause similar behaviour to that seen in rumination disorder. In situations like this, the person wouldn’t be given a separate diagnosis of rumination disorder, and the behaviour should be addressed as part of the treatment for the illness that caused it.
The number of people who have rumination disorder is unknown. Rumination disorder can lead to malnutrition, weight loss, dental erosions, and electrolyte disturbances if left untreated. It is therefore very important to contact your doctor as soon as possible if you’re worried about yourself or someone you know and to ask to be referred to a specialist who can rule out other causes for the behaviour and discuss appropriate treatment.
Possible signs of rumination disorder
- Vomiting food that has been partly digested on a regular basis
- No obvious physical illness that causes this behaviour
- Re-chewing and swallowing food that they have brought up
- Hiding their behaviour, for example, by coughing or covering their mouth
- Avoiding eating around others
- Avoiding eating before socialising
- Weight loss
- Malnutrition
- Not making expected weight gains
- Straining and arching the back with the head held back, making sucking movements with their tongue
- The appearance of finding the behaviour satisfying
- Being hungry and irritable between instances of bringing up their food
Pica
What is pica?
Pica is a feeding disorder in which someone eats non-food substances that have no nutritional value, such as paper, soap, paint, chalk, or ice. For a diagnosis of pica, the behaviour must be present for at least one month, not part of a cultural practice, and developmentally inappropriate – generally, it’s not diagnosed in children under the age of two, as it is common for babies to “mouth” objects, which can lead to them accidentally eating substances that are not meant to be eaten.
Often, pica is not revealed until medical consequences occur, such as metal toxicity, cracked teeth, or infections.
Pica affects people of all genders and ages, though it is more likely to first appear among children. It can occur alongside other illnesses, including other eating disorders. In cases where it is this other illness that has caused the behaviour related to pica, a separate diagnosis of pica would be made only if it is serious enough to need clinical attention beyond that already being provided for the other illness.
People with pica don’t usually avoid regular food, meaning they may still be getting all the nutrients they need. However, some non-food items that they consume can be very dangerous, especially if eaten in large quantities. If you’re concerned about yourself or someone else, you should visit your doctor as quickly as possible so that they can refer you for appropriate treatment.
The reasons that people develop pica are not yet clear, although several scientists have linked it to the nervous system, and have understood it as a learned behaviour or coping mechanism. In some cases, people with pica have been found to be deficient in certain minerals or vitamins, but this is often not the case.
The percentage of people who have it is not yet known, as different researchers may use different definitions of pica, leading to some confusion.
Nonetheless, it may be more likely to occur alongside:
Pregnancy
Iron deficiency anaemia
Intellectual developmental disorders
Depression
Obsessive-compulsive disorder and related disorders such as trichotillomania (hair-pulling) and excoriation disorder (skin-picking)
Schizophrenia
Some of the items that people may feel an urge to eat because of pica can be extremely harmful. If you or someone you know has eaten something that is not supposed to be eaten, you should seek medical help immediately. It may be necessary to contact the emergency services.
Possible signs of pica
Craving to consume substances that aren’t supposed to be eaten.
Eating substances that aren’t supposed to be eaten.
Physical illness as a result of eating harmful substances.
Diabulimia
Diabulimia is deliberate insulin underuse in people with type 1 diabetes for the purpose of controlling weight. About 38% of females and 16% of males with type 1 diabetes have disordered eating behaviors.
However, there is a serious health risk in this practice with the Insulin omission increasing the risk of retinopathy, neuropathy, and diabetic ketoacidosis. Within a longitudinal clinical study, diabulimia increased mortality risk threefold.
How are eating disorders treated?
It is essential to seek treatment early for eating disorders. Without treatment, up to twenty per cent (20%) of people with serious eating disorders die. (https://www.edreferral.com/statistics) People with eating disorders are at higher risk for suicide and medical complications.
Some people with eating disorders may also have other mental disorders (such as depression or anxiety) or problems with substance use.
Treatment plans for eating disorders include psychotherapy, medical care and monitoring, nutritional counselling, medications, or a combination of these approaches. Typical treatment goals include restoring adequate nutrition, bringing weight to a healthy level, reducing excessive exercise, and stopping binge-purge and binge-eating behaviours. Complete recovery is possible.
Accepting Help and Handling the Stigma of Eating Disorders

As if it is not enough to cope with both the psychological and physical symptoms, there is often a social stigma towards people with eating disorders that is greater than for other common mental health issues, like depression.
If you have an eating disorder, you may sense that others see you as weaker, responsible for your disorder or as someone who is using your disorder to get attention.
On the flip side, other women may express feelings of admiration or envy, particularly in the case of anorexia, seeing the condition as having some benefit in a society that values thin body types.
All of this can interfere with your motivation to get help for a condition that should not be considered desirable and is not your fault.
Getting a Diagnosis
If you think you or someone you know may have an eating disorder, it’s important for them to meet with a doctor or a therapist who specialises in eating disorders as soon as possible to get an assessment. A good therapist can also refer them to other specialists, if necessary.

Specific forms of psychotherapy (or “talk therapy”) and cognitive-behavioural approaches can be useful for treating specific eating disorders. The goal of psychotherapy and other types of counselling is to create a healthy relationship with food, your body and, ultimately, yourself;
Your first-aid manual will guide you throughout the various treatment available. It is not your job to make a diagnosis but to be aware of available treatments to offer the best results by preventing the situation escalating out of control and averting a death.
Research also suggests that medications may help treat some eating disorders and co-occurring anxiety or depression related to the eating disorder.
The SCOFF Questionnaire -test for detecting eating disorders
The SCOFF Questionnaire, devised by researchers at St George's Hospital Medical School, is a valid and reliable screening tool for detecting the existence of an eating disorder.
The questions focus on some key characteristics of anorexia and bulimia. (Which means this test is not appropriate to screen for binge eating disorder.) It is not intended to be used by the General public or MHFA to diagnose an individual but can act as a helpful guide to explore eating-related behaviours.
SCOFF Questionnaire
Do you make yourself sick because you feel uncomfortably full?
Yes | No
Do you worry you have lost control over how much you eat?
Yes | No
Have you recently lost more than one stone in a 3 month period?
Yes | No
Do you believe yourself to be fat when others say you are too thin?
Yes | No
Would you say that food dominates your life?
Yes | No
Interpretation of results
If you answer 'No' to every question, the test indicates you don't have an eating disorder. If you still think you may have an eating disorder, see your doctor.
If you answer 'Yes' to 1 question, with the rest answered as 'No', the test indicates you don't have an eating disorder. However, it does suggest you may have some issues with food or your body image.
If you are in any doubt about whether or not you have an eating disorder, see your doctor.
If you answer 'Yes' to at least 2 questions, the test indicates you may have anorexia nervosa or bulimia nervosa. This is not a diagnosis, but it is possible you have an eating disorder that needs further investigation by a qualified health professional. Please see your doctor.
Eating Disorder Statistics

Eating disorders general statistics:
At least 30 million people of all ages and genders suffer from an eating disorder in the U.S.
Every 62 minutes at least one person dies as a direct result from an eating disorder.
Eating disorders have the highest mortality rate of any mental illness.
13% of women over 50 engage in eating disorder behaviours .
In a large national study of college students, 3.5% sexual minority women and 2.1% of sexual minority men reported having eating disorder.
16% of transgender college students reported having eating disorder.
In a study following active duty military personnel overtime, 5.5% of women and 4% of men had an eating disorder at the beginning of the study, and within just a few years of continued service, 3.3% more women and 2.6% more men developed an eating disorder.
Eating disorders affect all races and ethnic groups.
Genetics, environmental factors, and personality traits all combine to create risk for an eating disorder.
Anorexia Nervosa:
0.9% of American women suffer from anorexia in their lifetime.
1 in 5 anorexia deaths is by suicide.
Standardized Mortality Ratio (SMR) is a ratio between the observed number of deaths in an study population and the number of deaths would be expected. SMR for Anorexia Nervosa is 5.86.
50-80% of the risk for anorexia and bulimia is genetic.
33-50% of anorexia patients have a comorbid mood disorder, such as depression. Mood disorders are more common in the binge/purge subtype than in the restrictive subtype.
About half of anorexia patients have comorbid anxiety disorders, including obsessive-compulsive disorder and social phobia.
Bulimia Nervosa:
1.5% of American women suffer from bulimia nervosa in their lifetime.
SMR for Bulimia Nervosa is 1.93.
Nearly half of bulimia patients have a comorbid mood disorder.
More than half of bulimia patients have comorbid anxiety disorders.
Nearly 1 in 10 bulimia patients have a comorbid substance abuse disorder, usually alcohol use.
Binge Eating Disorder (BED):
2.8% of American adults suffer from binge eating disorder in their lifetime.
Approximately half of the risk for BED is genetic.
Nearly half of BED patients have a comorbid mood disorder.
More than half of BED patients have comorbid anxiety disorders.
Nearly 1 in 10 BED patients have a comorbid substance abuse disorder, usually alcohol use.
Binge eating or loss-of-control eating may be as high as 25% in post-bariatric patients.
Other Specified Feeding or Eating Disorder (OSFED)
[Previously called Eating Disorder Not Otherwise Specified or EDNOS]:
OSFED, as revised in the DSM-5, includes atypical anorexia nervosa (anorexia without the low weight), bulimia or BED with a lower frequency of behaviours, purging disorder, and night eating syndrome.
SMR for EDNOS is 1.92.
Nearly half of EDNOS patients have a comorbid mood disorder.
Nearly 1 in 10 EDNOS patients have a comorbid substance abuse disorder, usually alcohol use.
Avoidant/Restrictive Food Intake Disorder (ARFID) :
ARFID is more than just “picky eating”. Children do not grow out of it and often become malnourished because of the limited variety of foods they will eat.
The prevalence of ARFID is still being studied but maybe 3-5% of children.
Boys might have a higher risk for this disorder than girls.
“Diabulimia:”
Diabulimia is a deliberate insulin underuse in people with type 1 diabetes for the purpose of controlling weight.
About 38% of females and 16% of males with type 1 diabetes have disordered eating behaviours .
Insulin omission increases risks for retinopathy, neuropathy, and diabetic ketoacidosis.
In a longitudinal study, diabulimia increased mortality risk threefold.
Sources:
https://anad.org/education-and-awareness/about-eating-disorders/eating-disorders-statistics/
First point of contact: Approaching the subject of an eating disorders

Listen and communicate non-judgmentally to the person
The way you discuss the person's issue may depend on their age, and for how long they have been dealing with eating disorder behaviours. Initially, focus on displaying empathy and not on changing the person or their perspective.
Discuss your concerns with them openly and honestly by reflecting the changes in their behaviour which concern you. Try to use “I” statements, such as "I am worried about you" rather than 'you' statements ("You are making me worried"), which may come across as accusing.
Try not to focus on weight or food, but rather the specific behaviours which concern you, as well as underlying emotional distress. Rather than talking about diets and weight loss, give the person room to discuss any feelings they may want to share. Do not comment positively or negatively about the person's appearance.
Be mindful that you may find it challenging to listen to what the person has to say, especially if you do not agree with what they are saying about themselves and food.
Be prepared that the person may be receptive to your attempt to reach out, but that there is also a good chance that they may deny that there is a problem. Even if you have approached them sensitively, they may become angry or defensive, or attempt to reassure you that all is well. Try to stay calm if this happens. It does not mean your conversation was not worth having. The person may require more time to absorb your concerns.
You may need to seek professional help on their behalf if you are concerned that there is a serious risk to their health or life. Wherever possible, try to include the person in such decisions and work with them.
Treatments that work for eating disorders
Treatment is rarely straightforward. Eating disorders may create multiple additional medical problems and can even be acutely life-threatening, requiring hospitalisation and forced nourishment. It often takes multidisciplinary teams of health professionals—including psychotherapists, medical doctors, and specialised dietitians or nutritionists—to bring about a full recovery.
Treatment for eating disorders usually involves addressing both disordered eating or exercise behaviours and physical consequences like weight loss and medical complications, as well as associated mental health issues like depression and anxiety.
Treatment should be tailored to individual needs, mainly where problems have existed for a while.
NICE guidelines recommend the following:
For anorexia nervosa:
- Usually, outpatient treatment involving specialist psychological support by an eating disorders team, lasting at least 6 months. Psychological approaches may include:
- Cognitive analytic therapy
- Cognitive behavioural therapy
- Interpersonal psychotherapy
- Psychodynamic therapy
- Family therapy
- Inpatient treatment may be required at times, if weight is dangerously low.
This should be in a specialist eating disorder setting and combine physical and psychosocial interventions.
Feeding a patient against their will is only used as a last resort.
- In addition to individual treatment, children and adolescents should also be offered family interventions (this may include therapeutic help involving the whole family, advice on managing behaviour and facilitating communication).
- Drug treatment (including antidepressants) needs to be carefully considered due to the increased risk of side effects due to low weight.
For bulimia nervosa:
- As a first step, patients should be encouraged to follow evidence-based self-help programmes. Alternatively, antidepressant drug treatment may help (usually SSRIs)
- Cognitive behavioural therapy for bulimia nervosa (CBT-BN) is a specifically adapted form of CBT and should be offered to adults over 4-5 months (16-20 sessions)
- As an alternative, interpersonal psychotherapy may be considered (longer duration of 8-12 months)
- Adolescents may also be treated with CBT-BN, and this may involve whole family approaches
- Inpatient treatment is usually only considered where there is serious risk of suicide or self-harm
It may be helpful to encourage the person to surround themselves with other people who are supportive of them. There are also specific organisations that provide help, support and information on eating disorders which may be of benefit. See the Helpful Resources below.

Self-help
While seeking professional help is important, don’t underestimate your own role in recovery. The more motivated you are to understand why you developed an eating disorder, and to learn healthier coping skills, the quicker you will see change and healing.
The following tips can help:
Learn healthier ways to cope with emotional pain
It may seem like eating disorders are all about food—after all, your rules and fears about dieting and weight have taken over your life. However, the food itself is not the real problem.
Disordered eating is a coping mechanism for stress or other unpleasant emotions. You may refuse food to feel in control, binge for comfort, or purge to punish yourself, for example. But whatever need your eating disorder fulfils in your life, you can learn healthier ways to cope with negative emotions and deal with life’s challenges.
The first step is figuring out what’s really going on inside.
Are you upset about something?
Depressed?
Stressed out?
Lonely?
Is there an intense feeling you’re trying to avoid?
Are you eating to calm down, comfort yourself, or to relieve boredom?
Once you identify the emotion you’re experiencing, you can choose a positive alternative to starving or stuffing yourself.
Here are a few suggestions to get you started:
Call a friend
Listen to music
Play with a pet
Read a good book
Take a walk
Write in a journal
Go to the movies
Get out into nature
Play a favourite game
Do something helpful for someone else
Avoid relapse
The work of eating disorder recovery doesn’t end once you’ve adopted healthier habits. It’s important to take steps to maintain your progress and prevent relapse.
Develop a solid support system.
Surround yourself with people who support you and want to see you healthy and happy. Avoid people who drain your energy, encourage disordered eating behaviours, or make you feel bad about yourself.
Identify your “triggers.
Are you more likely to revert to your old, destructive behaviours during the holidays, exam week, or swimsuit season? Or are difficulties at work or in your relationship likely to trigger your disordered eating habits?
Know what your early warning signs are, and have a plan for dealing with them, such as going to therapy more often or asking for extra support from family and friends.
Avoid pro-ana and pro-mia websites.
Do not visit websites that promote or glorify anorexia and bulimia. These sites are run by people who want excuses to continue down their destructive path.
The “support” they offer is dangerous and will only get in the way of your recovery.
Keep a journal.
Writing in a daily journal can help you keep tabs on your thoughts, emotions, and behaviors. If you notice that you’re slipping back into negative patterns, take action immediately.
Stick with your eating disorder treatment plan.
Don’t neglect therapy or other components of your treatment, even if you’re doing better. Follow the recommendations of your treatment team.
Fill your life with positive activities.
Make time for activities that bring you joy and fulfillment. Try something you’ve always wanted to do, develop a new skill, pick up a fun hobby, or volunteer in your community. The more rewarding your life, the less desire you’ll have to focus on food and weight.
If you do lapse, don’t beat yourself up.
Recovery is a process—and that often involves setbacks. Don’t let feelings of guilt or shame derail your recovery, but think about how you’ll handle the same situation next time.
Remember: One brief lapse doesn’t have to turn into a full-blown relapse.
Bibliography
Shih-Hsien L, et al. (2014). Serotonin and mental disorders: A concise review on molecular neuroimaging evidence. DOI:
10.9758/cpn.2014.12.3.196
Cowen PJ, et al. (2015). What has serotonin to do with depression? DOI:
10.1002/wps.20229
Dale E, et al. (2015). Emerging mechanisms and treatments for depression beyond SSRIs and SNRIs. DOI:
10.1016/j.bcp.2015.03.011
Depression: How effective are antidepressants? (2017).
ncbi.nlm.nih.gov/pubmedhealth/PMH0087089/
Clin Neuropharmacol. 2005 Sep-Oct;28(5):228-37.
Dopaminergic contribution to the regulation of emotional perception.
Salgado-Pineda P1, Delaveau P, Blin O, Nieoullon A.
https://www.psycom.net/midlife-eating-disorder-crisis/
Shih-Hsien L, et al. (2014). Serotonin and mental disorders: A concise review on molecular neuroimaging evidence. DOI:
10.9758/cpn.2014.12.3.196
Cowen PJ, et al. (2015). What has serotonin to do with depression? DOI:
10.1002/wps.20229
Dale E, et al. (2015). Emerging mechanisms and treatments for depression beyond SSRIs and SNRIs. DOI:
10.1016/j.bcp.2015.03.011
Depression: How effective are antidepressants? (2017).
ncbi.nlm.nih.gov/pubmedhealth/PMH0087089/
Clin Neuropharmacol. 2005 Sep-Oct;28(5):228-37.
Dopaminergic contribution to the regulation of emotional perception.
Salgado-Pineda P1, Delaveau P, Blin O, Nieoullon A.
https://www.psycom.net/midlife-eating-disorder-crisis/
Prevalence of Eating Disorders: A Comparison of Western and Non-Western Countries (2004) https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1435625/)
Prevalence of eating disorders over the 2000–2018 period: a systematic literature review
Marie Galmiche, Pierre Déchelotte, Grégory Lambert, Marie Pierre Tavolacci
The American Journal of Clinical Nutrition, Volume 109, Issue 5, May 2019, Pages 1402–1413, https://academic.oup.com/ajcn/article/109/5/1402/5480601
Why Intervention Is Necessary to Prevent Eating Disorder Deaths https://www.verywellmind.com/yes-eating-disorders-can-be-deadly-1138269
PsychGuides.com https://www.psychguides.com/eating-disorder/treatment/
Eating Disorder Treatment and Recovery https://www.helpguide.org/articles/eating-disorders/eating-disorder-treatment-and-recovery.htm
Eating Disorders: About More Than Food https://www.nimh.nih.gov/health/publications/eating-disorders/index.shtml
Mental Health First Aid (USA) https://www.mentalhealthfirstaid.org/external/2018/05/3-common-types-of-eating-disorders/
What’s the Difference Between Dopamine and Serotonin? https://www.healthline.com/health/dopamine-vs-serotonin
What has serotonin to do with depression? World Psychiatry. 2015 Jun; 14(2): 158–160.
The relationship between dopamine and serotonin https://www.medicalnewstoday.com/articles/326090.php#relationship
Eating disorders https://www.nhs.uk/conditions/eating-disorders/
Fat phobic and non-fat phobic anorexia nervosa: a comparative study of 70 Chinese patients in Hong
Kong (1993) https://www.cambridge.org/core/journals/psychological-medicine/article/fat-phobic-and-nonfat-phobic-anorexia-nervosa-a-comparative-study-of-70-chinese-patients-in-hong-kong/19F63570CD024570CED895F9AAE892B4
Christina Gregory - Orthorexia Nervosa https://www.psycom.net/eating-disorders/orthorexia/
CAMILA MENDES GETS REAL ABOUT HER STRUGGLE WITH AN EATING DISORDER http://www.mtv.com/news/3129249/camila-mendes-eating-disorder/
Taylor Swift praised for discussing eating disorder
https://www.bacp.co.uk/news/news-from-bacp/2020/24-january-taylor-swift-praised-for-discussing-eating-disorder/?fbclid=IwAR34vM2SzF9xMq3-2XugBkfTj7rkFn4McW1ZVNyVqFfWF6n0muzQK97wS0A
Eating Disorders https://www.psychologytoday.com/us/basics/eating-disorders
What has serotonin to do with depression? World Psychiatry. 2015 Jun; 14(2): 158–160.
(American Journal of Psychiatry, March 2017 https://www.sciencedaily.com/releases/2017/03/170301105554.htm)
Why Intervention Is Necessary to Prevent Eating Disorder Deaths https://www.verywellmind.com/yes-eating-disorders-can-be-deadly-1138269
PsychGuides.com https://www.psychguides.com/eating-disorder/treatment/
Eating Disorder Treatment and Recovery https://www.helpguide.org/articles/eating-disorders/eating-disorder-treatment-and-recovery.htm
ARFID & AUTISM https://www.arfidawarenessuk.org/the-link-with-autism-1
Recommended reading
If you want to seek help for a loved one with an eating disorder, three good resources are the Alliance for Eating Disorders Awareness,
- https://www.allianceforeatingdisorders.com/ which offers referrals to medical providers as well as other resources.
- The National Eating Disorders Association, https://www.nationaleatingdisorders.org. which has a helpline and information about various aspects of eating disorders. (USA)
- https://www.beateatingdisorders.org.uk/ Helpline 0808 801 0677 (UK)
Center Stage (2000 film) Star student Maureen (Susan May Pratt), a closet bulimic who seems poised for success, discovers that life is passing her by when she meets a pre-med student (Eion Bailey) who shows her the merits of a life without ballet, to the dismay of her controlling stage mother (Debra Monk), herself a failed ballet dancer and current ABC employee.
Case study- male anoxia https://www.nationaleatingdisorders.org/blog/running-away-manorexia
If you are concerned that you may have an eating disorder, this leaflet is designed to guide you
during a GP appointment and help you get a referral for specialist assessment.
https://www.beateatingdisorders.org.uk/uploads/documents/2017/10/gp-leaflet-website.pdf
Eating Disorder Organizations:
Glossary of Eating Disorder Terms
Approved Mental Health Practitioner
This role relates to the Mental Health Act 1983. If someone needs compulsory treatment, they will be involved in that decision. They act in the best interests of the patient and ensure that they understand their rights and are treated with dignity.
Cognitive Analytic Therapy (CAT)
Cognitive analytic therapy is a kind of therapy that can be recommended for the treatment of anorexia. It looks at past events that may explain the unhealthy thoughts that cause your anorexia and helps you to recognise and find ways to break the unhealthy patterns.
Cognitive Behavioural Therapy (CBT)
Cognitive behavioural therapy helps you to deal with problems by breaking them down into smaller parts. It focuses on current problems and how to change negative thought patterns to develop healthy ways of coping with them. This therapy is often recommended as part of the treatment for all kinds of eating disorders. It can be adapted to the needs of people with particular illnesses, such as bulimia (CBT-BN) or binge eating disorder (CBT-BED).
Counselling
A type of talking therapy where you can talk about your thoughts and feelings, which aims to help you overcome emotional issues that you’re struggling with.
CPN (Community Psychiatric Nurse) / CMHN (Community Mental Health Nurse)
A mental health nurse who may visit patients at home to support them as they go through treatment.
Dietician
A qualified health professional who can assess, diagnose and treat dietary problems. They are registered with a professional body, the Health and Care Professions Council.
Family therapy
Family interventions may be recommended for children and adolescents with eating disorders. This kind of therapy involves family members, acknowledging that the eating disorder can impact the people around the sufferer and helping them to better understand the illness.
Focal Psychodynamic Therapy (FPT)
This is a form of therapy based on the idea that mental health conditions may relate to past unresolved conflicts. The therapy encourages people to think about early events that may have impacted their mental health and helps them find healthy ways to cope with negative feelings.
General practitioner (GP)
Usually, the first port of call when seeking treatment for an eating disorder. They can assess your physical and mental health, give a diagnosis, prescribe treatment, and refer you for specialist care.
Interpersonal therapy (IPT)
This is a form of therapy that looks at the effect your relationship with others and with the outside world has on your mental health. It helps you to understand the feelings involved and develop healthy coping strategies. This can be part of the treatment for all kinds of eating disorders.
Modified Dialectical Behaviour Therapy (DBT)
This is a kind of therapy that focuses on your ability to control and regulate your emotional responses, and it can be adapted to help treat binge eating disorder.
Psychiatrist
A doctor who specialises in psychiatry, the field of medicine that involves the assessment, diagnosis and treatment of mental health conditions.
Psychologist
Someone trained in psychology, the study of how people think and behave. You might work with a clinical psychologist if you go through some form of therapy as part of your treatment. It’s advisable to check your psychologist is registered with the British Psychological Society.
Psychotherapist
Someone who is trained to deliver one or more types of therapy. You can see whether your psychotherapist is registered at the British Association of Counselling and Psychotherapy.
If you suspect that you or someone you know may be showing signs of one of these illnesses, then we strongly advise you to consult with a medical professional as quickly as possible so that they can give you more information and refer you for appropriate treatment. Remember, it is always best to seek treatment early.
There are also many other illnesses, both physical and psychological, that can lead to changes in someone eating behaviour, or in other areas that may be affected by an eating disorder, such as their feelings about their body.
If you’re worried about yourself or someone you know but do not feel that any of the disorders covered on this website accurately describe the symptoms you or they are experiencing, it’s always best to speak to a medical professional, who will be able to give you further advice.
UK
Beat is an excellent resource (beateatingdisorders.org.uk) for those affected by eating disorders. They provide a helpline (0808 801 0677 / 0711 for adults / under 18's) or email adults: help@beateatingdisorders.org.uk or under 18 to fyp@beateatingdisorders.org.uk. There is an online support groups, one to one web chats and more.
If you’re concerned that you may have an eating disorder, the following resource leaflet is designed to give you guidance during a GP appointment and help you get a referral for specialist assessment.






