- in Health and Wellness by Tony
- |
- 1 comments
Headache explained

One of the body’s most influential alarm signals is a headache, which is often a sign of physical or psychological overload. A headache occurs because of a primary or secondary cause.
Globally, it has been estimated that the prevalence among adults of current headache disorder is approximately 50%. Half to three-quarters of adults aged 18–65 worldwide have had a headache in the last year.
More...
Primary headaches
Migraine, or tension headaches, are among the most common primary headaches that lead people to seek medical treatment, and they affect an estimated 3 billion people each year.
This type of headache isn’t a symptom of any disease, but a condition on its own. It is a “primary headache“ because it is the main concern. Often, stress and disruptions in your sleep patterns cause these headaches.
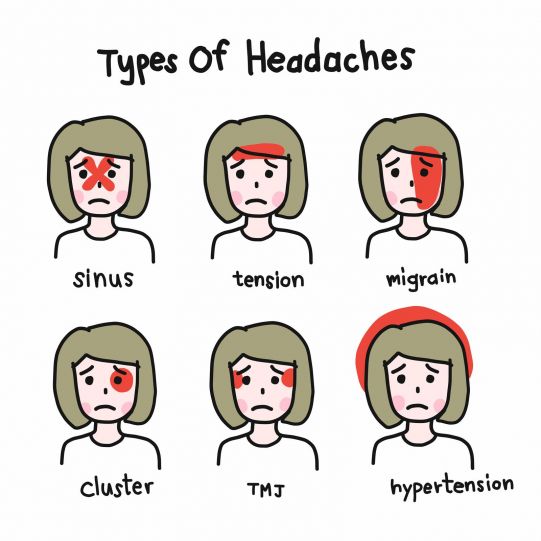
Secondary headaches
Secondary headaches manifest as a symptom of another health disorder. Different types of illnesses and disorders can cause a headache, including:
- Infection
- Medication Overuse
- High Blood Pressure
- Mental Health Conditions
- Head Injury or Trauma
- Stroke
- Tumour
- Nerve Disorders
- Sinus Congestion
Note: Only 1% of patients with a brain tumour will report a primary headache. If your primary headache is secondary, a healthcare provider must determine the cause of the pain and treat the disease to relieve the symptoms.
Headaches should not be ignored when accompanied by trauma to the head or neck, since any pain can signal a much more severe or even life-threatening ailment.
Overall, headaches are the most common medical complaint, lasting from a few minutes to hours or even days. Several types of headaches differ according to how and where the pain occurs.
These include tension headaches, simple headaches, cluster headaches, and migraines— an incredibly intense form that may frequently accompany nausea and impaired vision.
Various causes of headaches include stress, poor sleep habits, dehydration, lack of exercise, and certain medications. Headaches can also be triggered by allergies, colds, flu, sinus infections, and other conditions.

In many cases, there are several types of headaches, each of which is described below. Let’s begin with a quick overview of some of the most common types of headaches.
Simple headache
While many people don’t associate dehydration with headaches, some studies have shown that dehydration is a common cause. Even slight dehydration can alter a person’s function and thought patterns, making them feel worse.
Water can help the sufferer regain their hydration levels, and some studies have shown that drinking water can reduce the duration and intensity of headache pain. However, be cautious with this recommendation.
A study published in the Journal of Evaluation in Clinical Practice found that a single cup of water did not reduce the duration of headache pain.
Tension headache

Tension headaches are the most common type of headache, and they’re what we think of as typical, ‘every day’ headaches.
Tension headache pain tends to be:
Pain may occur across both sides and the front and back of the skull. In other words, your entire head may feel pain.
Stress can cause tight muscles in the shoulders and neck, which often leads to a tension headache, which starts in the neck and back and works its way up to feel like a tight band around your head.
People who suffer from tension headaches often feel stressed, with a persistent aches or stiffness; especially in their neck, upper back, or lower back and this tightness which is the trigger for a tension headache. There are many ways to relieve tension headaches, including stretching and relaxation techniques.
Stretching can also help release muscle tightness, triggering a tension headache. Try stretching after waking up, before going to sleep, and during breaks.
Increasing blood flow throughout your body helps prevent a build-up of muscle pain chemicals. Having a massage can help you to relieve stress as well as any related physical pains.
A thorough physical exam is necessary to rule out underlying medical conditions and other causes of a tension-type headache. If a headache occurs frequently or worsens, see a doctor, and they will perform a complete medical exam to rule out underlying conditions.
Chronic tension headaches can be signs of a severe medical ailment such as a brain tumour or weakened blood vessel, so make sure to schedule regular check-ups.
Migraine headache
Migraines are the second most common type of primary headaches and occur less often than tension headaches, which are usually much more severe. They are two to three times more common in women than men because of hormonal influences.
Small consolation if you are among 8% of all men who have migraines. About 20% of migraines begin with one or more neurological symptoms called an aura.
Visual complaints are most common, including halos, sparkles or flashing lights, wavy lines, and even temporary loss of vision. The aura may also produce numbness or tingling on one side of the body, especially the face or hand.
Some patients develop aura symptoms without getting headaches; they often think they are having a stroke, not a migraine.

A Harvard study reported that migraines boost the risk of heart attacks by 42%, so men with migraines should take their headaches to heart.
A simple headache can be mistaken for a migraine if there is no apparent cause. They may occur once or twice daily, lasting several hours to a day.
The symptoms of a migraine include pulsing pain in one side of the head. Symptoms may also include nausea, vomiting, and increased sensitivity to light or sound.
It is vital to seek immediate treatment for this type of headache, especially if it is frequent and continues to interfere with your life. One way to remember the features of migraine is to use the mnemonic word POUND.
Pulsating pain or throbbing varies with the heartbeat.
One to three days duration of severe untreated attacks
Unilateral location (one-sided) pain
Nausea and vomiting. Sensitivity to light or sound (Photophobia / Phonophobia).
Disabling intensity / Pain intensity is moderate to severe.
There’s no such thing as a universal migraine trigger. But some common triggers can cause or contribute to migraine episodes in some people.
Eating certain foods often triggers a migraine headache, and Migraines may be started by just one type of food.
Caffeine

Too much caffeine and experiencing caffeine withdrawal can cause migraine or headaches. Caffeine can cause side effects such as increased heart rate, anxiety, depression, sleep disturbances, restlessness and tremors.
But according to the American Migraine Foundation, caffeine can actually help stop oncoming migraine attacks.
Artificial Sweeteners

Many processed foods contain artificial sweeteners and sugar alternatives added to foods and drinks to add sweetness.
But these sweeteners can cause migraine, and Aspartame is thought to trigger migraine episodes.
Alcohol
Alcohol is one of the more common products thought to trigger migraine or a cluster headache, a stabbing pain in the eye that may last hours, go away, and come back several times daily.
Headaches are a common symptom of a hangover.
Alcohol is a diuretic and makes people need to urinate because it suppresses the release of a hormone called vasopressin. That can result in dehydration, which can cause a headache.
Sweating, vomiting, and diarrhoea are also symptoms of a hangover and can lead to further dehydration. Consuming non-alcoholic liquid or eating soup can help a person rehydrate and improve their headache.
According to one study, over 35% of the participants with migraine reported that alcohol was one of their common triggers. For some people, a few ounces of red wine are all it takes to provoke a headache, although any kind of alcohol can be a trigger.
Chocolate

According to the American Migraine Foundation, chocolate is thought to be the second most common trigger for migraine attacks, after alcohol. They say it affects an estimated 22 per cent of people who experience migraine.
Chocolate contains caffeine and beta-phenylethylamine, which may trigger headaches in some people.
Foods containing MSG

Monosodium glutamate (MSG) is a sodium salt of glutamic acid, which naturally exists in our bodies.
MSG is found in certain foodstuffs and many meals as a food additive. It’s considered safe to eat, but some researchers link it to migraine attacks.
The American Migraine Foundation notes that it may trigger severe migraine episodes in 15 per cent of those with migraine. Other preservatives may also be a trigger in some people.
Cured meats

Cured meats — including deli meats, ham, hot dogs, and sausages — contain preservatives called nitrates, which preserve colour and flavour.
These foods can release nitric oxide into the blood, which is thought to dilate blood vessels in the brain. There’s some evidence that nitric oxide can cause or contribute to migraine.
Aged cheeses

Studies on food and headaches date back to the 1920s; however, research on foods triggering migraines – specifically on foods containing tyramine – have been more common in recent years. Most of the research is based on diet manipulation and patient feedback.
In many cases, the amino acid can cause an increase in blood pressure and then trigger a migraine headache in tyramine-sensitive people.
Aged cheeses contain a substance called tyramine, which forms when a food’s ageing causes the breakdown of proteins. Tyramine is a naturally occurring compound that comes from the amino acid called “tyrosine.” It acts as a releasing agent that impacts our neurotransmitters.
The longer the cheese has aged, the higher the tyramine content. Typical cheeses that are high in tyramine include:
- feta
- blue cheese
- Parmesan
Pickled and fermented foods
Like ageing cheeses, above, pickled and fermented foods can contain high amounts of tyramine.
These foods include:
- pickles
- kimchi
- kombucha (which can also have alcoholic content)
- pickled okra
- pickled jalapeños
Frozen foods

Eating frozen foods and drinks like ice cream or slushies can trigger severe, stabbing pains in the head. You’re most likely to experience headaches that become migraine attacks if you’re gulping cold food quickly, exercising, or overheating.
Many frozen meals are high in sodium, some containing at least half of your daily sodium allotment per dish.
Salty foods
Table salt, known chemically as sodium chloride, is made up of 40% sodium.
There is growing evidence linking migraines with sodium. During a migraine, levels of sodium have been found to rise in cerebrospinal fluid, the liquid that bathes the brain and central nervous system. And sodium levels in this liquid seem to peak in the early morning and late afternoon – times of day when people commonly report experiencing migraines.
It’s estimated that at least half of people with hypertension have blood pressure that’s affected by sodium consumption — meaning they’re salt sensitive. In addition, your risk for salt sensitivity increases with age.
Ginger tea
As you may already know, various forms of ginger have been used to treat nausea for centuries, making it an appropriate choice for menstrual migraine. And while it doesn’t have to be tea to work, drinking something hot can be a soothing experience.
As far as clinical research goes, the evidence for ginger’s effectiveness has been inconclusive. So while you may not see a massive impact from this home remedy, it probably won’t hurt to try it.
Cluster headaches

Cluster headaches are uncommon but very severe and occur five times more often in men than women. Although anyone can get cluster headaches, the typical patient is a middle-aged man with a history of smoking.
Cluster headaches seem seasonal and often happen in the spring or Autumn. The problem gets its name because the headaches tend to come in clusters, with one to eight headaches a day during a one-to three-month period every year or two, often simultaneously.
The pain always strikes one side of the head and is very severe. The eye on the painful side is red and watery, the eyelid may droop, and the nose runs or is blocked.
The attack starts abruptly and lasts for 30 to 60 minutes. Most sufferers become restless and agitated during the episode, unable to sit still, pace, jog in place, or beat their heads against a wall.
Nausea and sensitivity to light and sound may accompany the pain. Sumatriptan is often effective for cluster headaches, particularly when given by injection. Inhaling high flow oxygen soon after the onset of the headache can often stop the attack.
Sinus headaches

Sinus headaches occur when the sinus passages behind your eyes, nose, cheeks, and forehead are congested, and this causes pressure and pain. You might experience a sinus headache from a sinus infection, which causes congestion and inflammation in the sinuses (open passageways behind the cheeks and forehead).
People, and even healthcare providers, often mistake migraines for sinus headaches.
Symptoms of sinus headaches include:
- Bad taste in my mouth.
- Deep, constant pain in your cheekbones and forehead.
- Facial swelling.
- A Sensation of fullness in the ears.
- Fever.
- Pain that gets worse with sudden head movement or straining.
- Mucus discharge (snot).
The pain of dental origin can be referred to in many areas of the head and face. Facial pain of dental origin is often caused by caries that progress to infection of the pulp or apical abscess or periodontal disease.
The international classification of Headache Disorders no longer uses the term “sinus headache” because the phrase was too broad. But the term is still widely used by doctors and patients.
According to the American Migraine Foundation, 50 per cent of migraine misdiagnoses start with a person thinking they have a sinus headache. Up to 90 per cent of people who go to the doctor for sinus headaches find out they have migraine instead.
Chronic myofascial pain
Chronic myofascial pain is most common and is similar to fibromyalgia. The pain is unilateral, dull, and localised to the preauricular region. Pain is exacerbated by chewing, yawning, or the stimulation of specific trigger points, usually found with palpable bands of muscle.
If your headache also includes having a fever and stiff neck, these are signs that you might have meningitis. Meningitis is a condition in which inflammation occurs in the spinal cord membranes and brain. You may also experience other symptoms, including muscle pain, vomiting, rash, and tiredness.
Meningitis can progress quickly and become life-threatening. If you experience these symptoms, seek immediate medical attention.
An otolaryngologist should be consulted for concerns of the head, neck or sinus-related headaches.
Facial pain with headaches
Headache and facial pain are common complaints in the emergency and outpatient setting. However, headaches and facial pain can have numerous other aetiologies that are important for the clinician to consider.
Hemicrania continua
Hemicrania continua is a chronic and persistent headache that always occurs on one side of the face and head. Additionally, people with the condition may experience periods of severe pain instead of the constant pain already felt, making this a debilitating headache.
Temporomandibular Joint (TMJ) Headache
The following is a simplified checklist of specific signs and symptoms you should watch out for as early indications of a Temporomandibular disorder (TMD).
- Your headache is more prevalent when you wake up in the morning or mid-afternoon.
- You frequently experience tension headaches.
- Your headache is more severe when you chew.
- Your headache is often in areas near your temples, under or over your eyes, in the ear and/or jaw area.
- You may experience pain in the ear, possibly accompanied by ringing or buzzing sounds.
- You hear clicking or popping noises when opening your jaw; in severe cases, your jaw may lock when you open your mouth, requiring manual assistance to close it.
- Your jaw opening is limited (a good reference of the standard opening is three fingers width).
- Your jaw muscles are sore or tender; you may find your back teeth to lack the strength to bite down hard.
- There is swelling on the sides of your face.
- You have sensitive teeth in the absence of dental problems.
- Your partner has told you that you grind your teeth at night.
- You find yourself clenching your teeth hard during the day, especially under stress. (Our lower jaw is usually 1-2 cm apart from our upper jaw in resting position under normal conditions.)
- Your upper and lower teeth do not align properly; you may have overlapping teeth, your upper teeth may not cover your lower teeth, or you may have an intense bite where you see very little of your bottom front teeth. (https://www.dpdental.com/tmj-headache/)
The menstrual cycle
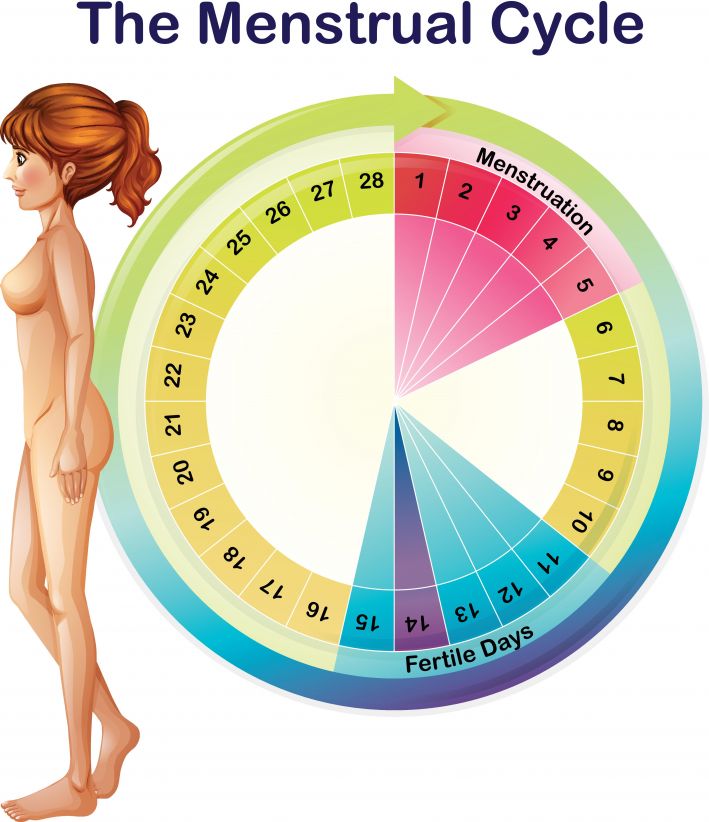
From painful cramps to persistent nausea, there’s not much to love about getting your period. And when you add menstrual migraine on top of all that, things can get unpleasant. The menstrual cycle has been linked to some types of headaches, specifically tension-type headaches and migraines.
Women are more likely than men to get migraine headaches, which researchers think is due to the influence of the hormones related to the menstrual cycle.
You get hit with migraine attacks at the same time every month—the drop in estrogen levels that happens before your period is triggering those painful headaches. Although doctors aren’t entirely sure why this happens, the hormonal connection is clear.
Treatment for menstrually-related headaches includes pain relief medication and hormonal therapy. The same hormone-stabilising effect that keeps you from getting pregnant also prevents that monthly estrogen drop, thereby sparing you the menstrual migraine (and your period, depending on which birth control you’re using). Birth control can help you avoid your period’s worst symptoms and migraine attacks.
Menstrual migraines are thought to be caused by a drop in hormones before the start of the period. Migraines that occur only with the beginning of the period are called Pure menstrual migraines.
In a study of women referred to headache specialists, about 1 in 10 of the participants stated that their migraines started at the time of menarche (the first menstrual period).
In one study, taking oral contraceptives affected migraines, with 24% of people experiencing increased frequency of migraines.
pregnancy

Headaches are common in pregnancy.
A 2021 review of studies estimated that 17 per cent of pregnant people experience primary headaches or migraine.
During pregnancy, you may experience stress and significant hormonal changes that lead to headaches. Some medications can be harmful to the mother or fetus. (also see study below)
Migraines may be triggered by stress, fatigue, or hormonal changes such as pregnancy. Migraines particularly hard hit women of childbearing age. However, experience shows that migraines become milder during pregnancy.
Migraines are now linked to elevated blood pressure, abortions, caesareans, preterm births and babies with low birth weight.
Published in the scientific journal Headache 2019 and carried out at the Department of Clinical Epidemiology, University and Aarhus University Hospital, Denmark.
The study also suggests that prescription migraine drugs may alleviate the complications.
Another important finding in that study was that the risk of caesarean sections is 15-25 per cent higher for pregnant women with migraine than pregnant women without migraine.
It also indicates that the migraine medication isn’t the cause of the complications, but rather the migraine itself.
Briquets syndrome
In the past, this disorder was thought to be related to emotional stress, and the pain was dismissed as being “all in their head”. However, patients with Briquet’s syndrome seem to experience pain or other symptoms that increase the level of pain.
Pain and worry create a cycle that is hard to break. People with a history of physical or sexual abuse are more likely to have this disorder. However, not every person with Briquet’s syndrome has a history of abuse.
As researchers study the connections between the brain and body, there is more evidence that emotional well-being affects how people perceive pain and other symptoms.
Research suggests genetic and environmental factors may contribute to the risk of developing this disorder, and it appears to affect women at a much higher rate than men. Briquet’s syndrome may originate from depression or anxiety, or as a response to severe psychosocial stress.
Seasonal allergies
Allergies that last an extended period can cause the sinuses to become inflamed, called rhinitis or hay fever.
Performing a spinal tap
In some cases, brain conditions like inflammation and bleeding may cause headaches. A lumbar puncture spinal tap involves using a long needle to draw cerebrospinal fluid from your spine to be analysed.
What is a COVID-19 headache?

A review in 2021 analysed headaches and their relationship with COVID-19. It discussed other recent studies estimating the prevalence of the symptom and found that headaches are present in 10 to 20 per cent of COVID-19 cases.
Even though there is still much to learn about the effects of COVID-19, researchers believe the virus may cause inflammation in the brain, leading to a headache. However, more research is needed to be sure.
“Panic attacks, irritability, headaches, muscle aches, increased heart rate, heart palpitations, increased blood pressure, breathing problems, upset stomach, insomnia, and chronic fatigue are all common effects of anxiety.”
— Dr. Lewis Jassey medical director at Leafwell
Over-the-counter pain relievers

If you get occasional headaches, you can take care of them yourself. Over-the-counter pain relievers such as:
Acetaminophen (Tylenol, other brands) and nonsteroidal anti-inflammatories (NSAIDs) such as aspirin, naproxen (Aleve, other brands), or ibuprofen (Motrin, Advil, other brands) often do the trick but follow the directions on the label, and never take more than you should.
Hot or cold compresses
Here’s an inexpensive remedy that reduces migraine and menstrual pain: hot and cold compresses. For migraine pain, you’ll want to apply them to the base of your neck or your temples. Disposable ice packs, while not the most environmentally friendly, can be kept by your bed instead of in the freezer, so you can skip the trip to the kitchen while you’re in pain.
A heating pad or warm shower may help; some people feel better with a short nap or light snack.
Cold compress Moisten a cloth with cold water, put two drops of peppermint oil on it and apply it to the painful area for about 15 minutes.
Potato poultice Cut two large unpeeled potatoes into quarters and boil until tender. Mash them and press out the excess moisture. Wrap the warm mixture in a cloth and carefully place it on the back of the neck. Let it remain until it cools, about 15 minutes.
No matter how you use your compresses, be sure to use them in moderation: The National Headache Foundation suggests capping cold packs used for 15 minutes at a time, to prevent ice burns and heating pads can cause skin burns or even fires if you don’t keep an eye on them.
Here are some more ways to relieve headaches naturally
1. Get plenty of rest. This is one of the best things you can do for your body to relieve headaches. If you have been working hard all day long without taking time off, then the chances are that you will feel tired. Get enough sleep, so your brain has time to recover.
2. Drink lots of water. Dehydration is another cause of headaches, and you will feel better when you drink more water because your body will not retain excess fluids.
3. Take an Epsom salt bath. The magnesium sulfate found in Epsom salts helps relax muscles and reduce pain, and it is also helpful in reducing swelling, soaking in a warm bath with Epsom salts.
Essential oils

We’re sure we’re not the first individual to suggest this favoured remedy to you. Still, we should note that despite all the gossip, there isn’t a lot of evidence that most essential oils actually do anything for all the conditions they’re supposed to treat.
The research suggests that some essential oils can help relieve headaches, including lavender, peppermint, and chamomile.
So, these oils may be an excellent place to start if you’re prone to hormonal headaches or migraine attacks. They can be inhaled or applied topically using a roll-on stick applicator, like Cove’s Essential Oil Roll-On. And like ginger, they’re unlikely to harm you—as long as potent scents aren’t a trigger.
Acupressure

Acupressure is all about applying pressure to specific points on your body, which is supposed to relieve pain, as well as nausea, anxiety, and even depression. While there isn’t much clinical evidence to back up all those claims, there’s plenty of anecdotal evidence that acupressure works.
Craniofacial therapy, also known as ‘cranial sacral therapy or CST, is a non-invasive alternative treatment that many massage therapists, chiropractors, and osteopaths use.
Cannabidiol

Here’s another option for migraine or period-induced nausea that’s a good choice for those who don’t mind trying a less-tested treatment. While there haven’t been any large-scale studies into whether CBD is effective for migraine pain in general, it has been shown to treat nausea.
CBD, or cannabidiol, is a natural substance found in the hemp plant, Cannabis sativa. Inevitably, people connect cannabis with marijuana, but while they come from the same family of plants, taking a CBD supplement and using marijuana are two very different things. Cannabidiol (CBD) and delta-9-tetrahydrocannabinol (THC) are the two predominant cannabinoids found in cannabis (marijuana).
If you’re going to try CBD, make sure you’re aware of the local laws in your state—most CBD products on the market right now aren’t being rigorously tested for safety (much less efficacy), so do your research before you buy anything.
Supplements

Are you looking for a natural option to prevent menstrual migraine?
Then supplements might be a better route for you. While ginger supplements can help with nausea (for the reasons mentioned above), riboflavin, CoQ10, and magnesium have the most clinical evidence for helping reduce the frequency and severity of migraine attacks (including hormonal ones). Magnesium supplements can also relieve symptoms of premenstrual syndrome.
There are alternative treatments that may help relieve sinus headaches. Bromelain, a mixture of enzymes found in pineapple juice, may thin nasal secretions. It has been suggested that stinging nettle (Urtica dioica) may relieve cases of long-standing rhinitis, but more research is needed.
If you have a severe sinus infection, it’s important to remember that these treatment methods won’t cure the condition or provide instant relief.
Prescription drugs
When prescription drugs are needed, most doctors turn to triptans, available as tablets, nasal sprays, or injections that patients can learn to give themselves. Examples include sumatriptan (Imitrex), zolmitriptan (Zomig), and rizatriptan (Maxalt).
Triptans provide complete relief within two hours for up to 70% of patients; the response is best if treatment is started early. Some patients require a second dose within 12 to 24 hours.
Other effective prescription drugs include beta-blockers (such as propranolol, nadolol and atenolol), certain antidepressants (such as amitriptyline), and certain anti-seizure medications (such as topiramate and valproate). Complex cases may benefit from referral to a headache specialist.
Intense pain
Another sign of a headache you shouldn’t ignore is intense pain. This means that you experience the worst pain of your life, which feels unbearable. If you experience a headache like this, you should not wait around.
Seek medical attention immediately. The intense pain is your body’s way of telling you something isn’t right. It might be a life-threatening condition like bleeding in the brain or an aneurysm.
Are headaches hereditary?
Genetics plays a role, since 70% of migraine victims have at least one close relative with the problem. Children with migraines usually have at least one parent who suffers from them, and kids whose parents have migraines are up to four times more likely to develop them.
Conclusion
If you are experiencing headache symptoms three or more times per month, it may be time to see a doctor. Also, consider seeking preventive treatment if the headaches impact your quality of life or cause additional problems like stress, depression, or other concerns.
Talking with your doctor if you are having new headaches or a different type of headache is also essential. Many common triggers for migraines, tension headaches, or cluster headaches have been discussed. The faster you identify them, the quicker you can resolve the issue and prevent unnecessary pain or discomfort.












[…] a clear medical explanation. People with SSD may experience pain, fatigue, abdominal discomfort, headaches, or other physical sensations that significantly impact their daily lives. They may also become […]